Medical billing and coding schools in West Virginia are growing at tremendous rates due to the increasing demand being reported by bls.gov. The time for enrollment could not be any better and we show you the correct path to coding and billing certification in WV. Lets not waste any more time and get started today!
How to become a medical billing and coding specialist in WV
The medical billing and coding field in West Virginia is regulated at a national level by the regulating bodies listed here.
Find Medical Billing and Coding Classes in West Virginia
What is the process for becoming a certified coder or biller in West Virginia?
The step by step easy process for becoming a medical biller or coder in West Virginia is detailed out in the following 4 steps.
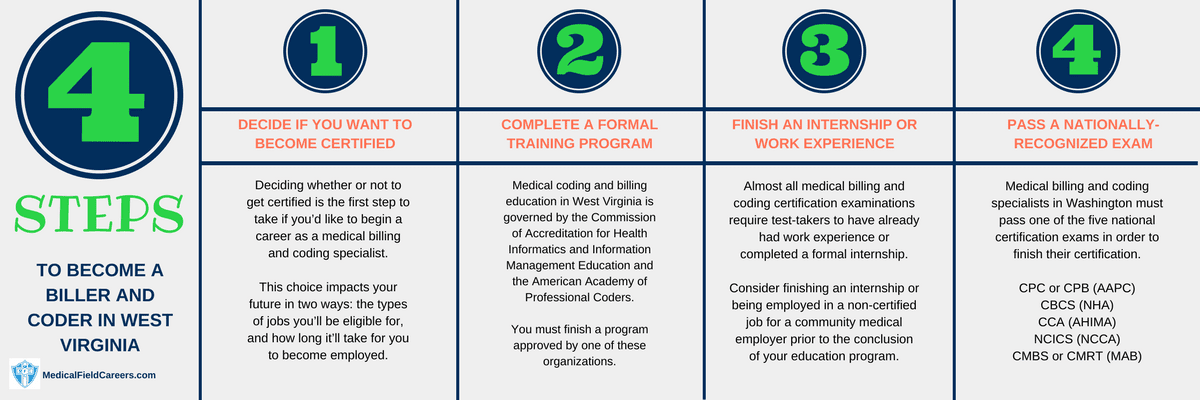
Step 1 – Do you want to get your certification?
The first step you should take is to decide whether or not you are going to become certified, and the specialized training it’ll require. Not only could this choice determine the roles you will be able to apply for, but it could also determine how much time it’ll take before you start working.
Step 2 – Complete a formal WV Medical Coding and Billing training program
You’ll find three different kinds of credentials that might be received by completing a professional medical billing and coding course – a diploma (or “certificate”, as they are also called), two-year associate degree, and a bachelor’s degree. Either type of credential is accepted by most employers, but you need to be cognizant of the benefits and drawbacks of each.
How to pick a coding and billing program in West Virginia
When selecting a program for your medical coding and billing education, being aware of what matters most to you is the most important factor. It can be cost or location or something else. But, just stick to what matters most and the best choice will present itself to you.
Approved Medical Coding and Billing Programs in West Virginia
The list below is of all the approved billing and coding programs in West Virginia.
Blue Ridge Community and Technical College 13650 Apple Harvest Drive Martinsburg WV 25403 304-260-4380
West Virginia Junior College-Morgantown 148 Willey St Morgantown WV 26505 304-296-8282
BridgeValley Community & Technical College 2001 Union Carbide Dr South Charleston WV 25136 304-734-6600
Huntington Junior College 900 Fifth Ave Huntington WV 25701 304-697-7550
West Virginia Northern Community College 1704 Market St. Wheeling WV 26003-3699 304-233-5900
Mountwest Community and Technical College One Mountwest Way Huntington WV 25701 866-710-3140
Ross Medical Education Center-Charleston 5707 MacCorkle Avenue S.E., Ste. 20 Charleston WV 25304-2816 304-925-5645
Ross Medical Education Center-Morgantown 1064 Suncrest Towne Centre Drive Morgantown WV 26505-1875 304-598-3689
Valley College-Princeton 617 Mercer Street Princeton WV 24740 304-425-2323
BridgeValley Community & Technical College 2001 Union Carbide Dr South Charleston WV 25136 304-734-6600
Valley College-Martinsburg 287 Aikens Ctr Edwin Miller Blvd Martinsburg WV 25404-6203 304-263-0979
Valley College-Beckley 120 New River Town Center Beckley WV 25801 304-252-9547
Step 3 – Do an internship or acquire job experience in West Virginia
Many of the coding and billing certification tests will require you to have finished an internship or acquire a specific amount of on-the-job experience before being approved to challenge the exam. Because of this, it’s strongly suggested that you either go through an internship or an entry-level non-certified position during your schooling.
Step 4 – Pass a Billing and Coding certification examination in West Virginia
Medical billing and coding specialists in West Virginia must pass one of the national certification examinations in order to finish their certification. These examinations are made up of segments on all major areas of knowledge you would have studied in your course.
Some of the major national certification exams administered in West Virginia are shown here.
Medical coding and salary salary and jobs in West Virginia
There’s a high demand for medical billing and coding specialists throughout est Virginia. Through the year 2024, the Bureau of Labor Statistics forecasts a 8% growth in additional opportunities for medical coding and billing specialists in West Virginia. The following record features data on medical coding and billing specialist salary in West Virginia by region.
| Location | Pay Type | Low | Median | High |
|---|---|---|---|---|
| United States | Hourly | $12.05 | $18.29 | $30.21 |
| Yearly | $25,070 | $38,040 | $62,840 | |
| West Virginia | Hourly | $10.85 | $16.11 | $25.57 |
| Yearly | $22,570 | $33,520 | $53,190 | |
| Washington-Arlington-Alexandria, DC-VA-MD-WV Metropolitan Division | Hourly | $12.74 | $20.32 | $34.86 |
| Yearly | $26,490 | $42,260 | $72,510 | |
| Morgantown, WV MSA | Hourly | $13.79 | $20.14 | $26.30 |
| Yearly | $28,670 | $41,900 | $54,710 | |
| Hagerstown-Martinsburg, MD-WV MSA | Hourly | $13.82 | $19.78 | $29.11 |
| Yearly | $28,740 | $41,140 | $60,550 | |
| Wheeling, WV-OH MSA | Hourly | $11.36 | $16.40 | $24.97 |
| Yearly | $23,630 | $34,100 | $51,940 | |
| Winchester, VA-WV MSA | Hourly | $11.45 | $15.82 | $24.84 |
| Yearly | $23,810 | $32,910 | $51,660 | |
| Charleston, WV MSA | Hourly | $10.44 | $15.24 | $23.18 |
| Yearly | $21,720 | $31,700 | $48,200 | |
| Huntington-Ashland, WV-KY-OH MSA | Hourly | $10.92 | $15.10 | $26.63 |
| Yearly | $22,720 | $31,400 | $55,390 | |
| North Central West Virginia BOS | Hourly | $10.69 | $15.01 | $25.03 |
| Yearly | $22,230 | $31,220 | $52,060 | |
| Southern West Virginia BOS | Hourly | $10.57 | $14.15 | $22.24 |
| Yearly | $21,990 | $29,430 | $46,260 |

